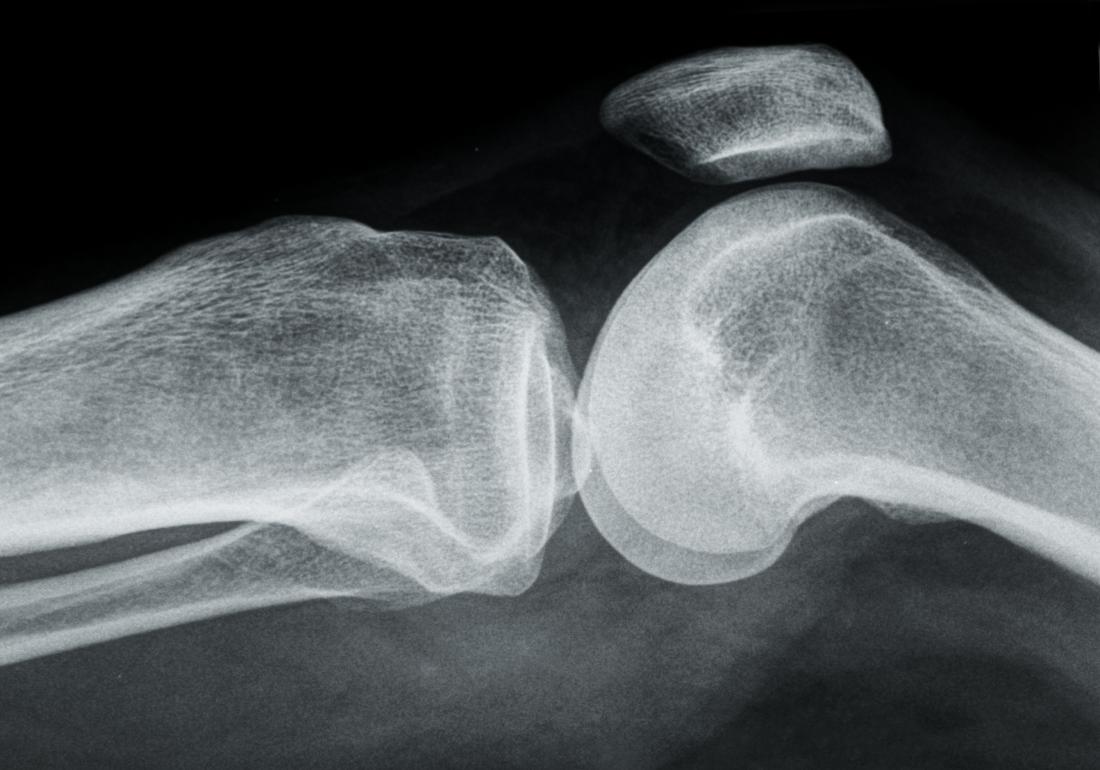
Osteoarthritis commonly affects knee joints.
Osteoarthritis is the most common arthritis type, causing pain and stiffness in the joints as cartilage steadily breaks down.
It is often referred to as “wear and tear” arthritis, as opposed to rheumatoid arthritis, which is caused by an immune response.
Most commonly affecting a person’s hands, knees, hips, feet, and spine, osteoarthritis symptoms tend to get worse over time.
Symptoms of joint swelling and tenderness can come and go over time — or, in some people, they can be constant. The degree of severity varies a great deal between individuals.
As the most common joint disorder in the United States, osteoarthritis affects over 30 million adults.
Several interventions can help manage osteoarthritis, including physical therapy, medications, and surgery. To date, however, nothing halts the progression of this debilitating condition.
It is still not exactly clear why cartilage continues to break down, and what mechanisms underpin the changes.
Risk factors for osteoarthritis include advancing age and obesity, so as the global population becomes older and heavier, the condition is likely to become increasingly prevalent.
Delving deeper into osteoarthritis
Recently, researchers led by Frederique Cornelis — from KU Leuven in Belgium — looked into the cellular changes involved in osteoarthritis and the interactions between certain proteins. Their findings are published in the journal Science Translational Medicine.
Specifically, the team was interested in ANP32A, which is a protein involved in a number of roles within cells, including intracellular transport and cell differentiation.
The researchers noted that levels of ANP32A were significantly lower in tissue samples from both humans and mice with osteoarthritis. This piqued their interest — so, using gene expression profiling, they dug a little deeper into the protein’s function.
They used a mouse model that is incapable of producing ANP32A, which causes them to develop osteoarthritis and osteopenia, or bone loss. They also developed a condition similar to cerebellar ataxia, symptoms of which include stumbling and a lack of coordination.
The study authors summarize their initial findings:
“ANP32A protects against the development and progression of osteoarthritis by preventing oxidative stress in the articular cartilage.”
Adding an antioxidant
Next, the researchers tested the effects of adding an antioxidant called N-acetyl-cysteine (NAC) to drinking water.
They found that adding NAC to the animals’ diet reduced symptoms of osteoarthritis, and cartilage damage seemed to be halted. Symptoms of cerebellar ataxia were also reduced.
To understand what mechanism might be behind ANP32A’s ability to reverse these symptoms, the researchers dug a little deeper. They found that ANP32A raises the levels of an enzyme known as ATM, which plays an important role in regulating cellular defensive responses against oxidative stress.
They explain, “ANP32A’s protective role can be attributed to promoting the expression of ATM in the articular cartilage, to preserve the cellular redox balance.”
In other words, if ANP32A is not present, there is less ATM available to mop up the free radicals that are causing damage to the cartilage.
The authors hope that understanding the role of ANP32A and ATM in more depth could lead to interventions for a number of difficult-to-treat and poorly understood conditions.
They believe that their findings “may have therapeutic implications not only in chronic joint disorders but also in bone and neurological diseases.”
However, there is much work still to do; as the authors make clear, this molecular interaction is unlikely to be the only mechanism involved in osteoarthritis. In the future, the team hopes to investigate other factors that might influence ANP32A production in cartilage.
