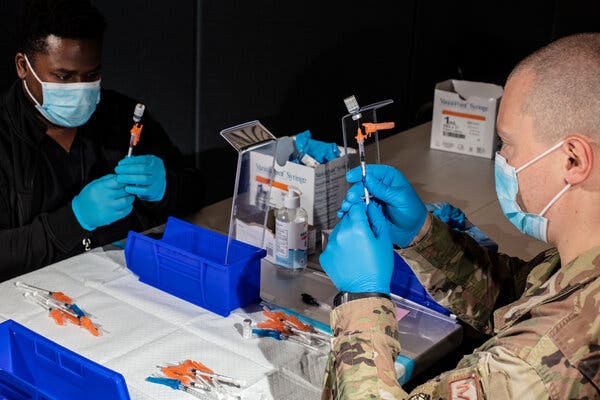
The Delta variant of the coronavirus can evade antibodies that target certain parts of the virus, according to a new study published on Thursday in Nature. The findings provide an explanation for diminished effectiveness of the vaccines against Delta, compared with other variants.
The variant, first identified in India, is believed to be about 60 percent more contagious than Alpha, the version of the virus that thrashed Britain and much of Europe earlier this year, and perhaps twice as contagious as the original coronavirus. The Delta variant is now driving outbreaks among unvaccinated populations in countries like Malaysia, Portugal, Indonesia and Australia.
Delta is now the dominant variant in the United States. Infections in this country had plateaued at their lowest levels since early in the pandemic, although the numbers may be rising, while hospitalizations and deaths related to the virus have continued a steep plunge. That’s partly because of relatively high vaccination rates: 48 percent of Americans are fully vaccinated, and 55 percent have received at least one dose.
But the new study found that Delta was barely sensitive to one dose of vaccine, confirming previous research that suggested that the variant can partly evade the immune system — although to a lesser degree than Beta, the variant first identified in South Africa.
French researchers tested how well antibodies produced by natural infection and by coronavirus vaccines neutralize the Alpha, Beta and Delta variants, as well as a reference variant similar to the original version of the virus.
The researchers looked at blood samples from 103 people who had been infected with the coronavirus. Delta was much less sensitive than Alpha to samples from unvaccinated people in this group, the study found.
One dose of vaccine significantly boosted the sensitivity, suggesting that people who have recovered from Covid-19 still need to be vaccinated to fend off some variants.
The team also analyzed samples from 59 people after they had received the first and second doses of the AstraZeneca or Pfizer-BioNTech vaccines.
Blood samples from just 10 percent of people immunized with one dose of the AstraZeneca or the Pfizer-BioNTech vaccines were able to neutralize the Delta and Beta variants in laboratory experiments. But a second dose boosted that number to 95 percent. There was no major difference in the levels of antibodies elicited by the two vaccines.
“A single dose of Pfizer or AstraZeneca was either poorly or not at all efficient against Beta and Delta variants,” the researchers concluded. Data from Israel and Britain broadly support this finding, although those studies suggest that one dose of vaccine is still enough to prevent hospitalization or death from the virus.
The Delta variant also did not respond to bamlanivimab, the monoclonal antibody made by Eli Lilly, according to the new study. Fortunately, three other monoclonal antibodies tested in the study retained their effectiveness against the variant.
In April, citing the rise of variants resistant to bamlanivimab, the Food and Drug Administration revoked the emergency use authorization for its use as a single treatment in treating Covid-19 patients.

The world’s known coronavirus death toll passed four million on Thursday, a loss roughly equivalent to the population of Los Angeles, according to the Center for Systems Science and Engineering at Johns Hopkins University.
It took nine months for the virus to claim one million lives, and the pace has quickened since then. The second million were lost in three and a half months, the third in three months, and the fourth in about two and a half months. The number of daily reported deaths has declined recently.
Those are officially reported figures, which are widely believed to undercount pandemic-related deaths.
“The numbers may not tell the complete story, and yet they’re still really staggering numbers globally,” said Jennifer B. Nuzzo, an epidemiologist at Johns Hopkins University’s Bloomberg School of Public Health.
Ms. Nuzzo said the number of excess deaths reported around the world suggested that “lower-income countries have been much harder hit than their official numbers would suggest.”
Dr. Tedros Adhanom Ghebreyesus, the director-general of the World Health Organization, called four million dead a tragic milestone on Wednesday, and said the toll was continuing to mount largely because of dangerous versions of the virus and inequities in the distribution of vaccines.
“Compounded by fast-moving variants and shocking inequity in vaccination, far too many countries in every region of the world are seeing sharp spikes in cases and hospitalizations,” Dr. Tedros said at a news conference.
The official death toll numbers tell only part of the horrifying pandemic story. In many places, people have died without family to comfort them because of rules to prevent the spread of the virus. And many countries were completely overrun.
The dead overwhelmed cremation grounds in India in May, where at least 400,000 confirmed deaths have been reported and the actual number is likely higher. That was also the case in funeral homes in the United States, which surpassed 600,000 known deaths last month.
Latin America ravaged
The virus has hammered Latin America since the start of the pandemic, and some of those nations have been grappling with their deadliest outbreaks to date.
As of Tuesday, seven of the 10 countries with the highest death rates relative to their populations over the past week were in South America, according to data from Johns Hopkins, and the virus has been a destabilizing force in many countries in the region.
Government health data in Colombia show that more than 500 people died from the virus each day in June. The country has also gone through weeks of explosive protests over poverty made worse by the pandemic that were sometimes met with a violent police response.
A wave of cases in Peru cost many people their livelihoods, and thousands of impoverished people occupied empty stretches of land south of Lima. In Paraguay, which as of Tuesday had the highest number of Covid-19 deaths per capita of any country during the previous week, social networks often resemble obituary pages.
Brazil, which recently passed 500,000 official deaths, had the highest number of new cases and deaths of any country in the past week. A recent study found that Covid-19 had led to a significant decrease in life expectancy in Brazil.
Vaccines make a difference
Several vaccines have proven effective against the coronavirus, including the highly contagious Delta variant, and death rates have dropped sharply in many parts of the world where large numbers of people have been vaccinated, like the United States and much of Europe.
But the virus is still running rampant in regions with lower rates of vaccination, like parts of Asia, Africa and South America. Some places with relatively high vaccination rates, like England, are also seeing spikes in cases, though fewer of those cases have been leading to hospitalizations and deaths.
Dr. Maria Van Kerkhove, who works on coronavirus response for the W.H.O., said that there were “more than two dozen countries that have epidemic curves that are almost vertical.”
“The virus is showing us right now that it’s thriving,” she said.
Wealthy countries and international organizations have pledged billions of dollars to Covax, a global vaccine-sharing initiative, and nations like the United States have promised to supply hundreds of millions of doses. But those numbers pale in comparison with the 11 billion vaccine doses that experts estimate will be needed to rein in the virus around the world.
To date, just under 3.3 billion vaccine doses have been administered worldwide, according to vaccination data from local governments compiled by the Our World in Data project at the University of Oxford. Nearly all have been of vaccines that require more than one dose to be fully effective.
Country-to-country differences in progress are stark, with some already inoculating most of their adult citizens while others have yet to report administering a single dose.

Africa has just had its “worst pandemic week ever,” the World Health Organization said on Thursday. The continent is short of vaccines, and the virus is sickening its young people and overwhelming its already fragile health care systems.
More than 251,000 new cases were reported in Africa in the week ending July 4, a 20 percent increase from the previous week, according to Dr. Matshidiso Moeti, the W.H.O. regional director for Africa.
For several weeks now, the continent has been experiencing a brutal wave of infections driven by the more contagious Delta variant, which is increasing hospitalization and fatalities, filling intensive-care beds, depleting oxygen supplies and pushing governments to institute new lockdown measures.
Sixteen African countries are reporting a resurgence in infections, with Malawi and Senegal added to the list this week. New case counts are doubling every 18 days, Dr. Moeti said, and have been rising for seven straight weeks.
“A few weeks ago, we projected this milestone would be reached shortly, and it brings me no joy to be right,” Dr. Moeti said at a news conference on Thursday. “For Africa, the worst is yet to come,” she warned, adding, “The end to this precipitous rise is still weeks away.”
A third wave of the pandemic is ripping through countries mainly in southern and eastern Africa, and one country in North Africa — Tunisia — is experiencing its fourth wave.
Namibia, a nation of just over 2.5 million people, has been recording more than 1,000 new cases a day, and several senior government officials have succumbed to the virus. A spike in cases in Zambia has pushed the government to restrict social gatherings and close schools.
In Uganda, which was praised for its initial coronavirus response, hospitals have been stretched thin, with some with patients racking up huge medical bills. Rwanda restricted movement in its capital late last month, and Kenya instituted partial lockdowns and extended curfew hours in over a dozen counties where the Delta variant was contributing to surges.
Many African countries continue to face challenges in detecting and sequencing virus variants, Dr. Moeti said. Testing and tracing remain limited as well: In a continent of 1.3 billion people, just over 54 million Covid-19 tests have been conducted, according to Dr. John Nkengasong, the director of the Africa C.D.C.
But the biggest challenge has been vaccination. With just over 53 million doses administered, only about 1 percent of Africa’s population is fully vaccinated.
African officials have accused wealthy nations of hoarding vaccine doses while millions of Africans remain vulnerable. Most African countries are dependent on the Covax vaccine-sharing initiative, which has been severely hampered by the Indian government’s decision in April to hold back doses manufactured there for domestic use and restrict exports.
As cases surge in Africa, some wealthy nations have begun donating vaccine doses to nations on the continent. And as more supplies come in, health officials are urging African countries to prepare to receive and administer the doses quickly.
“Governments and partners can do this,” Dr. Moeti said, “by planning to expand vaccination sites, improving cold chain capacities beyond capital cities, sensitizing communities to boost vaccine confidence and demand, and ensuring operational funding is ready to go when it is needed.”

Olympic organizers said on Thursday that they would bar spectators from most events at the Games scheduled to open in two weeks, a decision that followed the declaration of a new state of emergency in Tokyo in response to a sudden spike in coronavirus cases.
Officials have long insisted that they can hold the Tokyo Games safely amid a pandemic. Last month, they announced that they would allow domestic spectators at the events despite public fears that the Games could become a petri dish for new variants of the virus.
Now, the virus has again wreaked havoc on the planning of Olympic organizers, who gathered in an emergency meeting on Thursday night to decide how to respond to the latest challenge of a pandemic that had already delayed the Games by a year.
The announcement came only hours before the Olympic torch was set to begin the last — and long-delayed — leg of its trip through Japan. Officials decided this week that there would be almost no actual running during its two-week perambulation through Tokyo and its suburbs, replacing the marathon with a series of ceremonies that would be closed to the public.
Addressing reporters on Thursday night, Prime Minister Yoshihide Suga acknowledged the challenge the country faced as the more contagious Delta variant had begun to spread. He warned about the danger of the virus spreading beyond Tokyo as people traveled home for the summer holidays.
But at the same time, Mr. Suga pledged to deliver an Olympic Games that would go down in history not as another victim of the pandemic, but as an example of fortitude in the face of adversity.
Viewers will be tuning in from around the world, he said, and “I want to transmit to them a message from Tokyo about overcoming hardship with effort and wisdom.”

Richard Williamson, 86, was rushed from a Florida jail to a hospital last July. Within two weeks, he had died of Covid-19.
Hours after Cameron Melius, 26, was released from a Virginia jail in October, he was taken by ambulance to a hospital, where he died. The coronavirus, the authorities said, was a contributing factor.
And in New York City, Juan Cruz, 57, who fell ill with Covid while in jail, was moved from a hospital’s jail ward into its regular unit before dying.
None of these deaths have been included in official Covid mortality tolls of the jails where the men had been detained. And these cases are not unique. The New York Times identified dozens of people around the country who died under similar circumstances but were not included in official counts.
In some cases, deaths were added to facilities’ virus tolls after The Times brought missing names to the attention of officials. In other cases, people infected with the coronavirus while incarcerated were granted legal releases because of the severity of their illnesses but were not included in the death tallies of the jails where they got sick. Still other inmates’ deaths were left off facilities’ list of virus deaths for reasons that are unexplained.
More than 2,700 people are reported to have died of Covid-19 in connection to U.S. prisons, jails and immigration detention centers, but the additional cases raise the prospect that the known toll on incarcerated people falls far short of providing the full picture.
Concerns about how coronavirus deaths are documented have emerged throughout the pandemic, including a finding that the toll among nursing home residents in New York State was far higher than known because thousands who died in hospitals had not been included.
Public health officials say the prospect of overlooked virus deaths tied to the nation’s prisons, jails and immigration detention centers carries particular risks. It is challenging, the experts say, to prepare prisons for future epidemics without knowing the accurate toll. For now, the publicly known death totals connected to incarceration largely come from the facilities themselves.
“You can’t make good public policy if you don’t know what’s actually going on on the ground,” said Sharon Dolovich, director of the Covid Behind Bars Data Project at the University of California, Los Angeles, which tracks coronavirus deaths in American prisons.
Maura Turcotte, Rachel Sherman, Rebecca Griesbach, Ann Hinga Klein, Brendon Derr and

The assassination of President Jovenel Moïse of Haiti on Wednesday could complicate efforts to contain the Covid-19 pandemic in the Caribbean nation, which has yet to begin vaccinating its citizens, officials from the World Health Organization warned.
Carissa Etienne, the director of the Pan American Health Organization, which is part of the W.H.O., said her organization had made Haiti a priority in recent weeks as reported cases have surged.
“I am hopeful that the arrival of vaccines in the country can start to turn the tide of the pandemic and bring some relief to the Haitian people during these very difficult times,” Dr. Etienne said. “We continue to stand with them now and will redouble our efforts.”
Haiti did not experience the kind of surge early in the pandemic that many experts feared could devastate the country, the poorest in the Western Hemisphere. But the pandemic has grown worse in recent weeks, with a rise in reported cases that experts say is almost certainly an undercount, considering the country’s limited testing capacity.
Last month, Covid-19 claimed the life of René Sylvestre, the president of Haiti’s Supreme Court — a leading figure who might have helped to establish order in the wake of an assassination that has plunged the country into even deeper political uncertainty.
Dr. Etienne’s organization said in an email that while it was too soon to evaluate the impact of the assassination, “further deterioration of the security situation in Haiti could have a negative impact on the work that has been done to curtail Covid-19 infections,” as well as on vaccination plans.

The organization said that Haiti was also facing challenges from the start of hurricane season and the recent detection of the Alpha and Gamma virus variants on the island. Though “vaccines are expected to arrive shortly” in Haiti, the organization said it did not have a specific delivery date.
In June, Dr. Etienne urged the global community to do more to help Haiti cope with rising coronavirus cases and deaths. “The situation we’re seeing in Haiti is a cautionary tale in just how quickly things can change with this virus,” she said.
Haiti is an extreme example of the “stark inequities on vaccine access,” Dr. Etienne said. “For every success, there are several countries that have been unable to reach even the most vulnerable in their population.”
Across Latin America and the Caribbean, there are millions of people who “still don’t know when they will have a chance to be immunized,” she said.
She said the inequitable distribution of vaccines posed practical and moral problems.
“If we don’t ensure that countries in the South have the ability to vaccinate as much as countries in the North, this virus will keep circulating in the poorest nations for years to come,” Dr. Etienne said. “Hundreds of millions will remain at risk while the wealthier nations go back to normal. Obviously, this should not happen.”
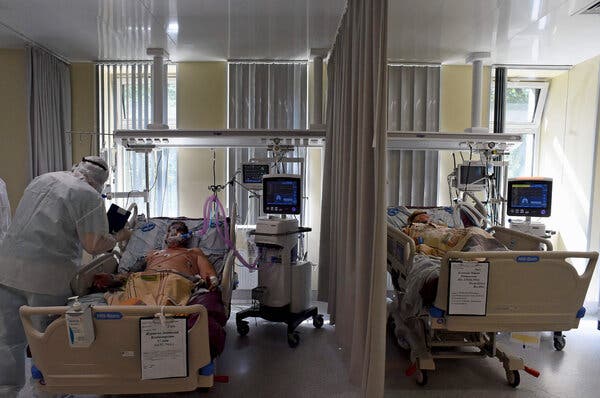
While highly effective Covid-19 vaccines were developed with unprecedented speed, the search for drugs to treat people infected with the coronavirus has lagged. Researchers hope that drugs already on the market for other diseases might be found to help Covid patients, but the challenge has been to identify the best candidates.
In a new article published in Nature on Thursday, an international group of researchers, led by Andrea Ganna of the Institute for Molecular Medicine in Helsinki, reported that when they scoured the genomes of nearly 50,000 people in 19 countries who had Covid-19, they found 13 genetic areas of interest that might focus the search for useful drugs.
The study cautioned that the genetic variations, which are inherited, could not themselves be used to predict who might contract Covid or, if infected with the coronavirus, who might become seriously ill.
Each of the genetic variations appears to be associated with a minuscule additional risk of infection or severe disease. But even so, a drug for another disease that directs its effects toward a gene variation that also occurs in some Covid patients might also prove to help the Covid patients, the reasoning goes.
The cases the researchers studied included people who were hospitalized with severe Covid, people whose electronic health record showed that they had a positive Covid test, and people who simply self-reported that they had had Covid infections.
Each genetic area found by the researchers represents small differences in a segment of DNA.
The most promising genetic variations, the researchers say, include those in a gene that has been previously reported as a risk factor for lung cancer. The variations result in increased expression of the gene in the lung and are associated with more severe Covid disease. The most severely affected Covid patients have trouble breathing, and some need respirators as the virus affects their lungs.
A second genetic variation, also associated with severe disease, is known to reduce the risk of developing autoimmune diseases but to increase the risk of tuberculosis.
The third genetic variation increases the risk of infection with the virus. This gene binds to a cell surface protein, ACE2, that the coronavirus uses to hitch itself to cells and enter them.
The possible significance of other variations is less clear. Not all are in genes themselves — some are in areas of DNA between genes.
The study’s authors caution in their paper that how important the research will be in finding Covid treatments remains to be seen.
“Future work will be required to better understand the biological and clinical value of these findings,” the authors wrote.

The highly contagious Delta variant of the coronavirus is now the dominant variant in the United States, accounting for 51.7 percent of infections, according to new estimates from the Centers for Disease Control and Prevention.
As health officials had expected, the Delta variant has rapidly overtaken Alpha, the variant that spread through the United States this spring. Alpha, first detected in Britain, now makes up just 28.7 percent of infections, according to the C.D.C.
Still, overall, the average numbers of new virus cases and deaths across the country, as well as hospitalizations, are significantly down from the devastating peaks during previous national surges.
Delta was first detected in India. Research suggests that most vaccines still provide good protection against it and remain highly effective at preventing hospitalizations and deaths.
In England, for instance, where the variant now causes almost all infections, case numbers have risen sharply in recent weeks, but hospitalization rates have increased more slowly and remain low. Next week, a final decision will be made about whether to lift most remaining restrictions in England, including mask rules, on July 19.
Studies suggest, however, that a single shot of a two-dose regimen provides only weak protection against Delta, and public health experts have been encouraging Americans to get fully vaccinated as soon as possible.
As of Wednesday, 67.2 percent of adults in the United States have had at least one vaccine dose, and 58.4 percent are fully vaccinated.
Still, vaccination coverage remains highly uneven, both in the United States and globally, and public health experts say Delta poses a serious threat to unvaccinated populations. On Tuesday, President Biden again urged Americans to get their shots, citing concerns about Delta. “It sounds corny, but it’s a patriotic thing to do,” he said.
Health experts say the Biden administration may need to take more aggressive action to encourage vaccination, including urging employers and schools to adopt vaccine mandates. As of Wednesday, administering about 0.73 million doses per day on average, about a 78 percent decrease from the peak of 3.38 million reported on April 13, according to federal data.
As for the virus itself, the country has been averaging fewer than 15,000 new coronavirus cases a day for nearly a month, the lowest levels since testing became widely available and a fraction of what was reported in January, when the nation routinely identified more than 200,000 cases in a day.
In recent days, however, the average number of new cases has started to trend slightly upward nationally, driven largely by localized outbreaks in places with low vaccination rates, including parts of Missouri, Arkansas and Nevada.
As the Delta variant has spreads across the globe, the World Health Organization recently reiterated its longstanding guidance that everyone, vaccinated or not, should wear masks as a precaution. In the United States, however, the C.D.C. has not changed its advice that those who are fully vaccinated can skip masks in most situations.
U.S. health officials have suggested that the W.H.O.’s blanket suggestion was informed by its global purview, since many countries have had far less access to vaccines than the United States.
In New York City, efforts to monitor the spread of the virus have been scaled back, reflecting a steadily low caseload and a sense held by many that the virus is less of a wide threat. More than 51 percent of residents are fully vaccinated, according to city data, though large parts of the city still have lower rates. Coupled with concerns about Delta, some public health experts and elected officials are worried that the city may be pulling back on its surveillance measures too soon.
On Tuesday, Jen Psaki, the White House press secretary, said that the Biden administration was unlikely to impose new national mitigation measures, even if cases rise.
“The states are going to have to make evaluations and local communities are going to have to make evaluations about what’s in their interests,” she said.
Mitch Smith and Sharon Otterman contributed reporting.

As Fiji battles one of the fastest-growing coronavirus outbreaks in the world, the Pacific Island’s Olympic team departed on Thursday for Tokyo on a freight plane.
Their fellow passengers? A shipment of frozen fish.
The coronavirus outbreak had thwarted plans to get the athletes to Japan on regular planes after almost all passenger flights from the country were suspended until the end of July. Only a select number of repatriation and freight flights have been allowed to depart.
The country has been pummeled by the Delta variant of the virus, with an average of 57 daily new cases per 100,000 people over the past two weeks, according to a New York Times database. Just over 6 percent of the population is fully vaccinated against the coronavirus.
So arranging travel was a “logistical challenge,” Lorraine Mar, the chief executive of the Fiji Association of Sports and National Olympic Committee, told The Associated Press. The solution: a freight plane hauling mostly frozen seafood, with just enough passenger space for the athletes and other officials.
It’s a sharp contrast to other Olympians’ flashier modes of transport: U.S. basketball players Devin Booker, Jrue Holiday and Khris Middleton may travel to Tokyo in a private plane because of scheduling conflicts, while members of the British Olympian squad departed from Heathrow Airport in London on Tuesday wearing matching tracksuits in their team’s colors.
Around midnight local time, about 50 athletes and officials from Fiji, including the country’s men’s and women’s sevens rugby squads, departed on the flight from Nadi, the principal international airport, to Tokyo ahead of the Summer Games.
Before boarding, team members spent 96 hours in isolation and took tests 72 hours ahead of their departure, in line with guidelines set by officials in Tokyo. One official with the Fiji Olympic team who tested positive for Covid-19 was withdrawn from the event.
Ahead of the team’s departure, the country’s National Olympic Committee posted a video showing masked well-wishers brandishing Fiji’s sky-blue flag as they waved goodbye.
The country will compete in six sports, including archery, judo and table tennis. In 2016, 60 years after the country first competed in the Olympics, Fiji won its first medal when the men’s rugby team triumphed at the inaugural Olympic rugby sevens tournament in Rio de Janeiro.



